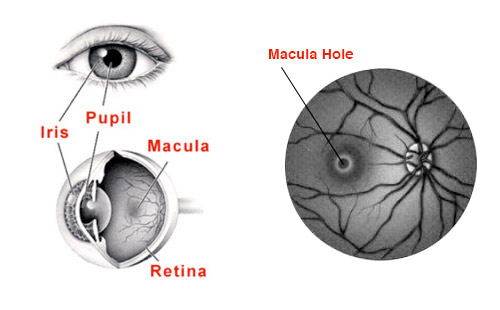
The retina is a thin layer of nerve tissue which lines the back of the eye. The macula is the most sensitive portion of the retina and is responsible for the high definition central vision required for tasks such as reading, watching television, using a computer and driving.
A macula hole is a small hole in this area of the retina caused by degenerative changes in the vitreous, which is the jelly like substance which fills the back portion of the eye. The symptoms of a macula hole are blurred central vision with or without some distortion. You may battle to read with this eye and will often have difficulty in judging distances and may find activities like climbing steps or pouring a drink difficult.

 A macula hole requires surgery to repair and this is performed by removing the vitreous (jelly) from the back of the eye (a vitrectomy) and filling the eye with gas, which will push the edges of the hole together and close the hole. Surgical success (closure of the hole) is achieved in 90% of patients with one surgery.
A macula hole requires surgery to repair and this is performed by removing the vitreous (jelly) from the back of the eye (a vitrectomy) and filling the eye with gas, which will push the edges of the hole together and close the hole. Surgical success (closure of the hole) is achieved in 90% of patients with one surgery.